





Published on Mar 04, 2023
Pradhan Mantri Ayushman Yojana PMJAY 2019 2020 Sarkari DNA Online : Under the ambit of Ayushman Bharat, a Pradhan Mantri Jan Arogya Yojana (PM-JAY) to reduce the financial burden on poor and vulnerable groups arising out of catastrophic hospital episodes and ensure their access to quality health services was conceived. PM-JAY seeks to accelerate India’s progress towards achievement of Universal Health Coverage (UHC) and Sustainable Development Goal - 3 (SDG3).
Pradhan Mantri Jan Arogya Yojana (PM-JAY) will provide financial protection (Swasthya Suraksha) to 10.74 crore poor, deprived rural families and identified occupational categories of urban workers’ families as per the latest Socio-Economic Caste Census (SECC) data (approx. 50 crore beneficiaries). It will have offer a benefit cover of Rs. 500,000 per family per year (on a family floater basis).
PM-JAY will cover medical and hospitalization expenses for almost all secondary care and most of tertiary care procedures. PM-JAY has defined 1,350 medical packages covering surgery, medical and day care treatments including medicines, diagnostics and transport.
To ensure that nobody is left out (especially girl child, women, children and elderly), there will be no cap on family size and age in the Mission. The scheme will be cashless & paperless at public hospitals and empanelled private hospitals. The beneficiaries will not be required to pay any charges for the hospitalization expenses. The benefit also includes pre and post-hospitalization expenses. The scheme is an entitlement based, the beneficiary is decided on the basis of family being figured in SECC database. When fully implemented, the PM-JAY will become the world’s largest government funded health protection mission.
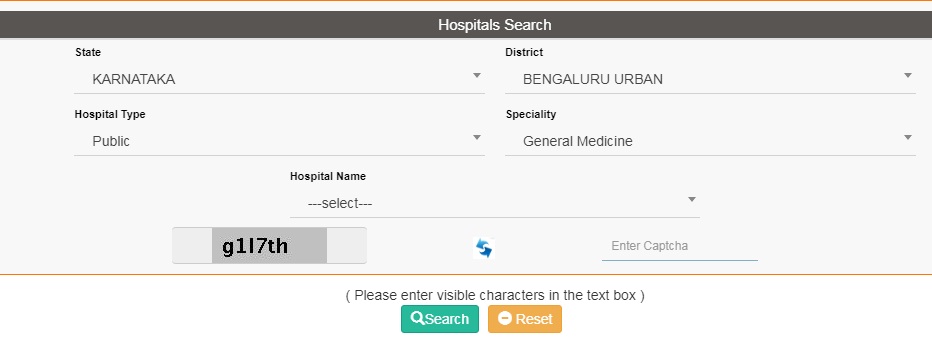
For the list of Hospitals, Kindly click the below link and Type as follows.
Visit https://hospitals.pmjay.gov.in/Search/empnlWorkFlow.htm?actionFlag=ViewRegisteredHosptlsNew
1. Select State
2. Select District
3. Select Hospital Type - Public, Private (Not for Profit) or Private(For Profit)
4. Select Speciality - General Medicine, Paediatric medical management, Neo-natal, Paediatric cancer, Emergency Room Packages, etc ......
5. Enter Captcha as shown
6. Lastly Enter Search.
Now you will get the list of Hospitals which is covered by Ayushman Bharat.
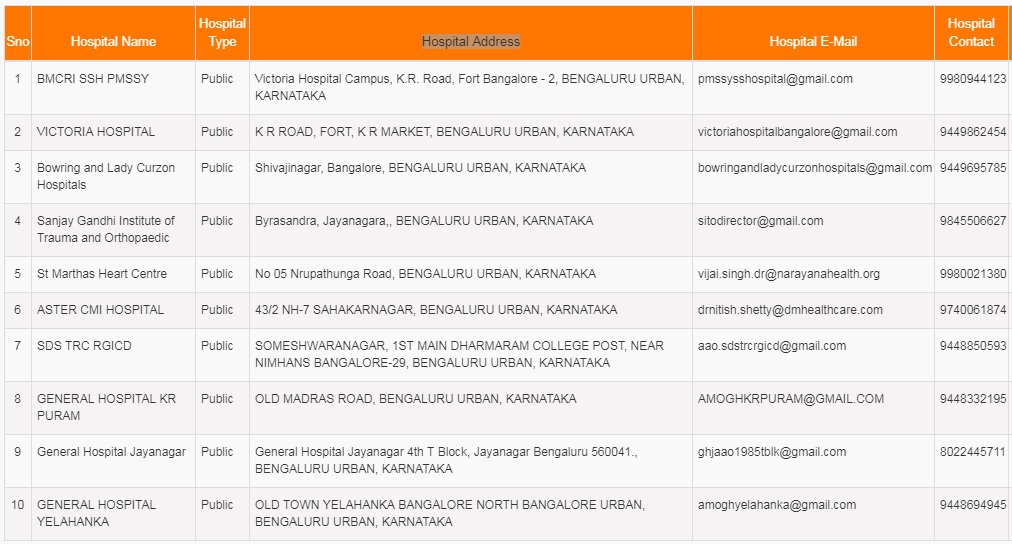
AB-NHPM will be rolled out across all States/UTs in all districts with an objective to cover all the targeted beneficiaries.
Ayushman Bharat or Pradhan Mantri Jan Arogya Yojana is National Health Protection Scheme, which will cover over 10 crore poor and vulnerable families (approximately 50 crore beneficiaries) providing coverage upto 5 lakh rupees per family per year for secondary and tertiary care hospitalization. Ayushman Bharat - National Health Protection Mission will subsume the on-going centrally sponsored schemes - Rashtriya Swasthya Bima Yojana (RSBY) and the Senior Citizen Health Insurance Scheme (SCHIS).
Ayushman Bharat (AB) is an attempt to move from sectoral and segmented approach of health service delivery to a comprehensive need-based health care service. Ayushman Bharat aims to undertake path breaking interventions to holistically address health (covering prevention, promotion and ambulatory care), at primary, secondary and tertiary level. Ayushman Bharat adopts a continuum of care approach, comprising of two inter-related components.
The first component, pertains to creation of 1,50,000 Health and Wellness Centres which will bring health care closer to the homes of the people. These centres will provide Comprehensive Primary Health Care (CPHC), covering both maternal and child health services and non-communicable diseases, including free essential drugs and diagnostic services. The first Health and Wellness Centre was launched by the Hon’ble Prime Minister at Jangla, Bijapur, Chhatisgarh on 14 April 2018. The second component is the Pradhan Mantri Jan Arogya Yojana (PM-JAY) which provides health protection cover to poor and vulnerable families. The Health and Wellness Centres will play a critical role in creating awareness about PM-JAY, screening for non-communicable diseases, follow-up of hospitalisation cases among others.
• Ayushman Bharat - National Health Protection Mission will have a defined benefit cover of Rs. 5 lakh per family per year.
• Benefits of the scheme are portable across the country and a beneficiary covered under the scheme will be allowed to take cashless benefits from any public/private empanelled hospitals across the country.
• Ayushman Bharat - National Health Protection Mission will be an entitlement based scheme with entitlement decided on the basis of deprivation criteria in the SECC database.
• The beneficiaries can avail benefits in both public and empanelled private facilities.
• To control costs, the payments for treatment will be done on package rate (to be defined by the Government in advance) basis.
• One of the core principles of Ayushman Bharat - National Health Protection Mission is to co-operative federalism and flexibility to states.
• For giving policy directions and fostering coordination between Centre and States, it is proposed to set up Ayushman Bharat National Health Protection Mission Council (AB-NHPMC) at apex level Chaired by Union Health and Family Welfare Minister.
• States would need to have State Health Agency (SHA) to implement the scheme.
• To ensure that the funds reach SHA on time, the transfer of funds from Central Government through Ayushman Bharat - National Health Protection Mission to State Health Agencies may be done through an escrow account directly.
• In partnership with NITI Aayog, a robust, modular, scalable and interoperable IT platform will be made operational which will entail a paperless, cashless transaction.
1. Households living in only one room with kucha walls and kucha roof.
2. Households with no adult member between age 16 to 59
3. Female headed households with no adult male member between age 16 to 59
4. Households having at least one disabled member and no able-bodied adult member
5. SC/ST households
6. Landless households deriving major part of their income from manual casual labour
7. Households without shelter
8. Destitute/ living on alms
9. Manual scavenger families
10. Primitive tribal groups
11. Legally released bonded labour
• Beggars;
• Rag-pickers;
• Domestic workers;
• Street vendors/cobblers/hawkers/other service providers working on the streets;
• Construction workers/ plumbers/ masons/ labor/ painters/ welders/ security guards/coolies and other head-load workers;
• Sweepers/ sanitation workers/ malis;
• Home-based workers/ artisans/handicrafts workers/ tailors;
• Transport workers/ drivers/ conductors/helpers to drivers and conductors/cart pullers/ rickshaw pullers;
• Shop workers/ assistants/ peons in small establishments/ helpers/ delivery assistants / attendants/ waiters;
• Electricians/ mechanics/ assemblers/repair workers;
• Washer-men/ chowkidars;
• Other work/non-work ;
• Non-work (pension/ rent/ interest, etc.) .
The beneficiaries will not be required to pay any charges and premium for the hospitalisation expenses. The benefit also include pre- and post-hospitalisation expenses.
Each empanelled hospital will have an 'Ayushman Mitra' to assist patients and will coordinate with beneficiaries and the hospital. They will run a help desk, check documents to verify the eligibility, and enrolment to the scheme.
Also, all the beneficiaries will be given letters having QR codes which will be scanned and a demographic authentication will be conducted for identification and to verify his or her eligibility to avail the benefits of the scheme.
Benefits of the scheme are portable across the country and a beneficiary covered under the scheme will be allowed to take cashless benefits from any public/private empanelled hospitals across the country.
There is no enrolment process in AB-NHPM as it is an entitlement-based mission. Families who are identified by the government on the basis of deprivation and occupational criteria using the SECC database, both in rural and urban areas, are entitled for AB-NHPM. Currently the database is based on census for the year 2011.
A list of eligible families has been shared with the respective state governments as well as state level departments like the ANMs, BMO, and BDOs of relevant areas. A dedicated AB-NHPM family identification number will be allotted to eligible families. Only families whose name is on the list are entitled for the benefits of AB-NHPM.
Additionally, families with an active RSBY cards as of 28 February 2018 will covered. No additional new families can be added under AB-NHPM. However, names of additional family members can be added for those families whose names are already on the on the SECC list.
The official website of AB-NHPM is www.abnhpm.gov.in . One may visit the site to view and download the beneficiary eligibility and empanelled hospitals list as and when it gets updated.
Services under the scheme can be availed at all public hospitals and empaneled private health care facilities. Also, the basic empanelment criteria allows empanelment of a hospital with a minimum of 10 beds, with the flexibility providprovided to states to further relax this if required. Empanelment of the hospitals under AB-NHPM will be conducted through an online portal by the state government. Information about empaneled hospitals will be made available through different means such as government websites and mobile apps. Beneficiaries can also call the helpline number at 14555.
To control costs, the payments for treatment will be done on package rate (to be defined by the Government in advance) basis. However, hospitals with NABH/NQAS accreditation can be incentivised for higher package rates subject to procedure and costing guidelines.
1. Government provides health insurance cover of up to Rs. 5,00,000 per family per year.
2. More than 10.74 crore poor and vulnerable families (approximately 50 crore beneficiaries) covered across the country.
3. All families listed in the SECC database as per defined criteria will be covered. No cap on family size and age of members.
4. Priority to girl child, women and and senior citizens.
5. Free treatment available at all public and empaneled private hospitals in times of need.
6. Covers secondary and tertiary care hospitalization.
7. 1,350 medical packages covering surgery, medical and day care treatments, cost of medicines and diagnostics.
8. All pre-existing diseases covered. Hospitals cannot deny treatment.
9. Cashless and paperless access to quality health care services.
10. Hospitals will not be allowed to charge any additional money from beneficiaries for the treatment.
11. Eligible beneificiares can avail services across India, offering benefit of national portability. Can reach out for information, assistance, complaints and grievances to a 24X7 helpline number - 14555
1. Go to NHA portal and Log in to mera.pmjay.gov.in
2. Enter your mobile number and captcha code.
3. A one-time password will be sent to your mobile number.
4. After entering the OTP, you will be taken to this screen.
5. Select the state: Fill all the fields like name, mobile number, ration card number, or Rashtriya Swasthya Bima Yojna URN number.
6. If your name is there in the list, it will show up on the right-hand side of the page.
7. Click on 'Family Members' tab to find the beneficiary details
• Respective special category certificates
• Age proof documents
• Family structure
• Identification details
• Contact information
• Scanned copy of Aadhar
• Income certificate
• Caste certificate
RSBY was launched in the year 2008 by the Ministry of Labour and Employment and provides cashless health insurance scheme with benefit coverage of Rs. 30.000/- per annum on a family floater basis [for 5 members], for Below Poverty Line (BPL) families, and 11 other defined categories of unorganised workers. To integrate RSBY into the health system and make it a part of the comprehensive health care vision of Government of India, RSBY was transferred to the Ministry of Health and Family Welfare (MoHFW) w.e.f 01.04.2015. During 2016-2017, 3.63 crore families were covered under RSBY in 278 districts of the country and they could avail medical treatment across the network of 8,697 empanelled hospitals. The NHPS comes in the backdrop of the fact that various Central Ministries and State/UT Governments have launched health insurance/ protection schemes for their own defined set of beneficiaries. There is a critical need to converge these schemes, so as to achieve improved efficiency, reach and coverage.