





Published on Nov 30, 2023
Virtual surgery, in general is a Virtual Reality Technique of simulating surgery procedure, which help Surgeons improve surgery plans and practice surgery process on 3D models.
The simulator surgery results can be evaluated before the surgery is carried out on real patient. Thus helping the surgeon to have clear picture of the outcome of surgery. If the surgeon finds some errors, he can correct by repeating the surgical procedure as many number of times and finalising the parameters for good surgical results. The surgeon can view the anatomy from wide range of angles. This process, which cannot be done on a real patient in the surgery, helps the surgeon correct the incision, cutting, gain experience and therefore improve the surgical skills.
The virtual surgery is based on the patient specific model, so when the real surgery takes place, the surgeon is already familiar with all the specific operations that are to be employed.
The first step in this is to generate a 3D model of the part of the body that undergo surgery Simulating human tissues-beit tooth enamel, skin or blood vessels-often starts with a sample from a flesh and blood person that is we should have a 3D model of the part of the body. Using computer graphics we first construct a reference model. Depending on this simulation needed, anatomical images can be derived from a series of patient's Magnetic Resonance Images (MRI), Computed Tomography (CT) or video recording, which are 2D images. These images are segmented using various segmentation methods like SNAKE'. The final model is obtained by deforming the reference model with constraints imposed by segmentation results. The image is digitally mapped on to the polygonal mesh representing whatever part of the body on organ is being examined. Each vortex of the polygon is assigned attributes like colour and reflectivity from the reference model.
For the user to interact with the graphics there must be software algorithms that can calculate the whereabouts of the virtual instrument and determines whether it has collide with a body part or anything else. The other thing is, we should have algorithms to solve how it looks or behave when the body part is cut. We need models of how various tissues behave when cut, prodded, punctured and so on. Here VR designers often portray the tissue as polygonal meshes that react like an array of masses connected by springs and dampers. The parameters of this model can then be tweaked to match what a physician experiences during an actual procedure. To create graphic that move without flickering collision detection and tissue deformation must be calculated at least 30 times/sec.
Advances in medical graphic allows ordinary medical scan of a patient anatomy be enhanced into virtual 3D views-a clear advantage for surgeon who preparing to do complicated procedures. Scans from MRJ and CT produces a series of things slices of the anatomy divided into volume data point or voxels, these slices are restacked and turned into 3D images by a computer. These 3D images are color enhanced to highlight, say bone or blood vessels.
The VR simulator basically consists of a powerful PC which runs the software and an interfacer- haptic interfacer- for the user to interact with the virtual environment. Usually the haptic interfacer works on force feedback loop.
The force feedback systems are haptic interfaces that output forces reflecting input forces and position information obtained from the participant. These devices come in the form of gloves, pens, joystick and exoskeletons.
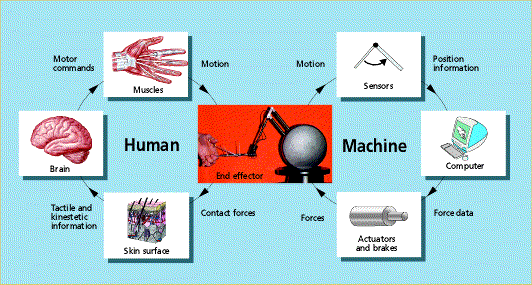
The figure (5.1) shows a haptic feedback loop, how human sense of touch interacting with a. VR system. A human hands moves the end effecter-shown here with haemostat-of a haptic device causing the device to relay its position via sensors to a computer running a VR simulation.
The computer determines what force should oppose that collision and relays force information to actuators or brakes or both, which push back against the end effecter. In the left hand loop, forces on the end effecter are detected and relayed to user’s brain. The brain, for example, commands the muscle to contract, in order to balance or overcome the force at the end effecter.
In medical applications, it is important that the haptic devices convey the entire spectrum of textures from rigid to elastic to fluid materials. It also essential that force feedback occur in real time to convey a sense of realism.
The rest of the system consists mostly of off-the-shelf components. The haptic device’s driver card plugs into usually a 500MHz PC equipped with a standard graphic card and a regular colour monitor. The software includes a database of graphical and haptic information representing the surgery part. The graphics, including deformation of virtual objects is calculated separately from the haptic feedback, because the latter must be updated much more frequently.
Tele-surgery allows surgeons to operate on people who are physically separated from themselves. This is usually done through a master-slave robot, with imaging supplies through video cameras configured to provide a stereoscopic view. The surgeon relies on a 3D virtual representation of the patient and benefit from dexterity enhancement afforded by the robotic apparatus’ prototype tele manipulator has been used to successfully perform basic vascular and urologic procedures in swine’s. More advanced system has been used to perform Coronary Anastomosis on exvivo swine hearts and in human undergoing endoscopic Coronary Artery Bypass grafting.
The second step in the simulation of surgery is simulating haptic-touch sensation. Physicians rely a great deal on their sense of touch for everything from routine diagnosis to complex, life saving surgical procedure. So haptics, or the abili to simulate touch, goes a long way to make virtual reality simulators more life like.
It also add a layer of technology that can stump the standard microprocessor. While the brain can be tricked into seeing seamless motion by flipping through 30 or so images per second, touch signals need to be refreshed up to once a millisecond. The precise rate at which a computer must update a haptic interface varies depending on what type of virtual surface is encountered-soft object require lower update rates than harder objects.
A low update rate may not prevent a users surgical instrument from sinking into the virtual flesh, but in soft tissues that sinking is what is expected. If we want something to come to an abrupt
stop that is in the case of born, etc it requires a higher update rates than bumping into something a little squishy like skin, liver etc.
But still, simulating squish is no easy task either. The number of collision point between a virtual squishy object and a virtual instrument is larger and more variable than between a virtual rigid object and an instrument. Most difficult to simulate is two floppy objects interacting with each other-such as colon and sigmoidocope, the long bendable probe used to view the colon-because of multiple collision point. In addition, the mechanics of such interaction are complicated, because each object may deform the other.
For simulating touch sensation, we have to calculate the forces applied to cut, prodde, puncture the various tissues. Also how they react or behave when cut, prodded, punctured using surgical instruments. First we have to make physical models of various tissues. The major difficulty in modeling organs is the physical behavior as they have all kinds of complexities-they are anistropic, non homogeneous and nonlinear. In addition, a great deal more physical measurement of tissues will be needed to make realistic haptic maps of complicated parts of the body such as abdomen.
Physical model is made assuming that tissues are polygon meshes that interact like an array of masses connected by springs and dampers. The parameter values are derived using complex nonlinear equations. The reaction forces are also calculated.
In coming years, VR designers hope to gain a better understanding of true mechanical behavior of various tissues and organs in the body. If the haptic device is to give a realistic impression of say pressing the skin on a patient’s arm, the mechanical contributions of the skin, the fatty tissue benefit, muscle and even bone must be summed up. The equations to solve such a complex problem are known, but so far the calculations cannot be made fast enough to update a display at 30Hz, let alone update a haptic interface at 500-1000Hz.
| Are you interested in this topic.Then mail to us immediately to get the full report.
email :- contactv2@gmail.com |