





Published on Nov 30, 2023
In microwave ablation, electromagnetic energy would be delivered via a catheter to a precise location in a coronary artery for selective heating of a targeted atherosclerotic lesion. Advantageous temperature profiles would be obtained by controlling the power delivered, pulse duration, and frequency.
The major components of an apparatus for microwave ablation apparatus would include a microwave source, a catheter/transmission line, and an antenna at the distal end of the catheter .The antenna would focus the radiated beam so that most of the microwave energy would be deposited within the targeted atherosclerotic lesion. Because of the rapid decay of the electromagnetic wave, little energy would pass into, or beyond, the adventitia. By suitable choice of the power delivered, pulse duration, frequency, and antenna design (which affects the width of the radiated beam), the temperature profile could be customized to the size, shape, and type of lesion being treated.
For decades, scientists have been using electromagnetic and sonic energy to serve medicine. But, aside from electro surgery, their efforts have focused on diagnostic imaging of internal body structures-particularly in the case of x-ray, MRI, and ultrasound systems. Lately, however, researchers have begun to see acoustic and electromagnetic waves in a whole new light, turning their attention to therapeutic-rather than diagnostic-applications. Current research is exploiting the ability of radio-frequency (RF) and microwaves to generate heat, essentially by exciting molecules. This heat is used predominantly to ablate cells. Of the two technologies, RF was the first to be used in a marketable device. And now microwave devices are entering the commercialization stage. These technologies have distinct strengths weaknesses that will define their use and determine their market niches. The depth to which microwaves can penetrate tissues is primarily a function of the dielectric properties of the tissues and of the frequency of the micro waves.
The tissue of the human body is enormously varied and complex, with innumerable types of structures, components, and cells. These tissues vary not only with in an individual, but also among people of different gender, age, physical condition, health and even as a function of external in puts, such as food eaten, air breathed, ambient temperature, or even state of minds. From the point of view of RF and Microwaves in the frequency range 10 MHz ~ 10GHz, however biological tissue can be viewed macroscopically in terms of its bulk shape and electromagnetic characteristic: dielectric constant and electrical conductivity . These are dependent on frequency and very dependent on the particular tissue type.
All biological tissue is somewhat electrically conductive, absorbing microwave power and converting it to heat as it penetrates the tissue. Delivering heat at depth is not only valuable for cooking dinner, but it can be quite useful for many therapeutic medical applications as well. These includes: diathermy for mild orthopedic heating, hyperthermia cell killing for cancer therapy, microwave ablation and microwave assisted balloon angioplasty. These last two are the subject of this article. It should also be mention that based on the long history of hi power microwave exposure in human, it is reasonable certain that, barring overheating effects, microwave radiation is medically safe. There have been no credible reported carcinogenic , muragenic or poisonous effects of microwave exposure.
Electromagnetic radiation begins with a phenomenon that occurs when electric current flows through a conductor, such as a copper wire. The motion of the electrons through the wire produces a field of energy that surrounds the wire and floats just off its surface. This floating zone or cloud of energy is actually made up of two different fields of energy, one electric and one magnetic. The electric and magnetic waves that combine to form an electromagnetic wave travel at right angles to each other and to the direction of motion.
If the current flowing through the wire is made to oscillate at a very rapid rate, the floating electromagnetic field will break free and be launched into space. Then, at the speed of light, the energy will radiate outward in a pulsating pattern, much like the waves in the pond. It is theorized that these waves are made up of tiny packets of radiant energy called photons. Streams of photons, each carrying energy and momentum, travel in waves like an undulating string of cars on a speeding roller coaster.
There is a very important difference between these radiations. As illustrated by the frequency spectrum on the right, microwaves used in microwave ovens, similar to microwaves used in radar equipment, and telephone, television and radio communication, are in the non-ionizing range of electromagnetic radiation. Non-ionizing radiation is very different from Ionizing radiation . Ionizing radiation is extraordinarily high in frequency (millions of trillions of cycles per second). It is, therefore, extremely powerful and penetrating. Even at low levels, ionizing radiation can damage the cells of living tissue. In fact, these dangerous rays, have enough energy and intensity to actually change (ionize) the molecular structure of matter. In sufficient doses, ionizing radiation can even cause genetic mutations. As shown on the frequency spectrum, the ionizing range of frequencies includes X-rays, gamma rays, and cosmic rays. Ionizing radiation is the sort of radiation we associate with radioactive substances like uranium, radium, and the fall-out from atomic and thermonuclear explosions.
Non-ionizing radiation is very different. Because of the lower frequencies and reduced energy, it does not have the same damaging and cumulative properties as ionizing radiation. Microwave radiation (at 2450 MHz) is non-ionizing, and in sufficient intensity will simply cause the molecules in matter to vibrate, thereby causing friction, which produces the heat that cooks the food.

Balloon angioplasty ( or Percutaneous Transluminal Coronary Angioplasty) has become one of the most commonly performed major cardiac operations in the United States. Compared to other surgical procedure, balloon angioplasty is relatively simple. A Special Catheter with a collapsed narrow inflatable balloon is inserted into a vein through an incision in the neck or leg and fed through blood vessels until it reaches the diseased arteries of the heart. Fluid is then pumped into the balloon inflating it to several times its nominal diameter. The enlarged tip quickly compresses the layer of plaque which is clogging the artery, leaving a much wider opening for blood flow. The balloon is then deflated and it is withdrawn with the catheter. The procedure avoids cardiac bypass surgery, or other more traumatic operation, and has been very successful at both extending and improving the quality of life.
Unfortunately, abrupt reclosure occurs in 3-5 % of the cases in which the balloon angioplasty is used and gradual restenosis of the artery occurs in 17-34% of the cases. Fiber optic guided laser light has been used to irradiate and thermally fuse fragmented plaque pieces following coronary angioplasty . Beneficial welding effects have been obtained for tissue temperature between 95 – 135 C. Although these previous studies have used laser radiation to deliver power to plaque, it is concluded that welding is primarily a thermal process dependent in maintaining an elevated temperature level. If sufficient heat can be delivered to the plaque it will become thermally fixed in place and compressed against the artery wall. However when using laser energy it is difficult to determine the proper laser intensity and length of exposure. Physicians must be extremely careful to avoid burning the healthy artery tissue and perforating the blood vessel wall. Insufficient exposure results in poor welding while too much injures the sensitive coronary artery.
An alternative physical process which can quickly deposit power in conductive media is microwave irradiation. Since the artherosclerotic plaque , which collects on the inner walls of the blood vessels, is composed of lipids and calcium particles, it can be considered LWC tissue. The healthy blood vessel wall out side the plaque layer is mostly muscle like HWC tissue. The challenge of microwave assisted balloon angioplasty (MABA) is to sufficiently heat the plaque layer without over heating the surrounding vessel wall. In addition, since plaque occlusions occur asymmetrically, it is essential to show that the electric field intensity and the deposited power are also concentrated in this LWC tissue layer even when it is predominantly on one side of the artery.
MABA devices were first reported by Rosen and subsequently studied. A patent was granted in 1991 which described a variety of antennas incorporated within and surrounding a catheter balloon. These applications made use of vary narrow antennas that could easily be guided through blood vessels into coronary arteries, and they relied primarily on field attenuation in the plaque layer to avoid harming the healthy artery wall. Since coaxial cables are commonly used as microwave transmission lines, they are naturally suitable to connect a microwave antenna to a power source in a catheter based applications.
The first reported MABA applications were dipoles and small radius helices, which tends to radiate with electric fields aligned parallel to their axes and thus, the artery wall. With this orientation, more power tends to be deposited in the healthy tissue than in the outer plaque surface, it is important to avoid overheating the artery wall, if possible. Understanding the role played by the wave polarization has led to an alternative MABA application design which minimizes the heating of healthy tissue.
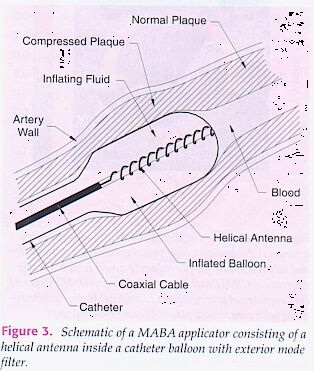
A reasonable choice is a helix designed to radiate a rapidly oscillating radially polarized field, positioned inside the balloon. Figure 3 shows the relative positions of this helical antenna as part of an angioplasty balloon in the blood vessel. This helical antenna has been analytically studied using a modal analysis based on the sheath helix model. While the sheath helix model does not consider launching or termination of waves, it does provide guidance in the choice of pitch angle and general concept feasibility .To ensure that the electric fields radiated into the plaque are most nearly radially–oriented , a mode filter ,composed of circumferential thin metallic traces on the expanded balloon, is used . This filter eliminates the dominant circumferentially directed electric field, which deposits power unfavorably in the healthy artery wall.
| Are you interested in this topic.Then mail to us immediately to get the full report.
email :- contactv2@gmail.com |