What are the signs and symptoms of Ramsay Hunt syndrome? How is it treated?
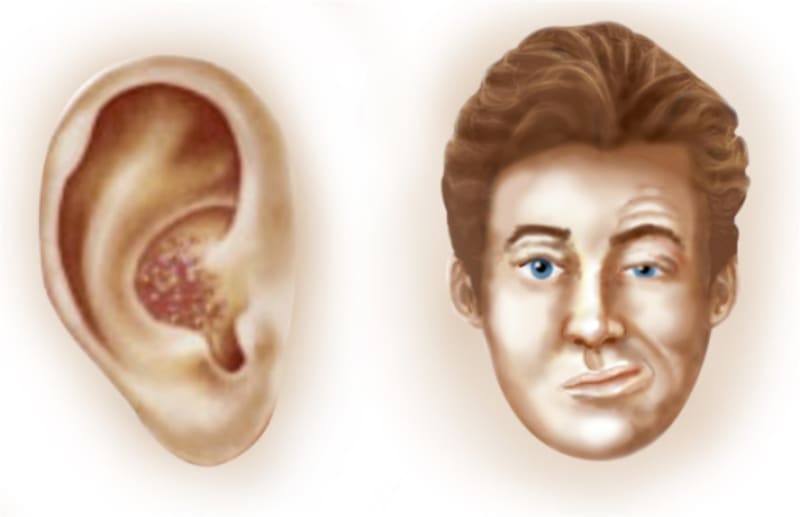
The Mayo Clinic says that Ramsay Hunt syndrome (also called herpes zoster oticus) happens when shingles affect a facial nerve near one of your ears. In addition to the painful rash, Ramsay Hunt syndrome can cause facial paralysis and hearing loss in the affected ear.
The same virus that causes chickenpox also causes Ramsay Hunt syndrome. After you get over chickenpox, the virus stays in your nerves. It could start up again years later. If it does, it can hurt the nerves in your face.
When Ramsay Hunt syndrome is treated right away, the chance of complications, such as permanent facial muscle weakness and loss of hearing, is lower.
The condition will go away on its own, but treatment aims to shorten the total length of the illness, relieve pain, and prevent complications that can happen. This activity talks about the role of the interprofessional team in figuring out what’s wrong with someone with Ramsay Hunt syndrome and how to treat it.
Epidemiology
Ramsay Hunt syndrome affects both people with healthy immune systems and people with weak immune systems. It happens to about 5 out of every 100,000 people every year, while Bell palsy happens to about 15 to 30 out of every 100,000 people every year. About 7 percent of cases of acute facial paralysis are caused by Ramsay Hunt syndrome, and about 10 percent of those are caused by zoster sine herpete.
People who don’t have strong immune systems are more likely to get sick and recover less completely. Ramsay Hunt syndrome can happen to anyone, and there have been cases in people as young as 3 months old and as old as 82 years old, though people in their 70s and 80s are most likely to get it. Stress, chemotherapy, immune system problems, infections, malnutrition, and other things that raise the risk of herpes zoster also raise the risk of Ramsay Hunt syndrome.
Treatment
Herpes zoster usually gets better on its own. So, the main goals of treatment are to lower the risk of late complications like spastic facial paralysis and postherpetic neuralgia. Using oral antivirals and steroids has been shown in more than one study to reduce long-term complications by a large amount. It is not clear, though, if these medicines shorten or lessen the severity or length of acute symptoms.
Researchers have looked into and found that acyclovir, valacyclovir, and famciclovir all work. Most of the time, the least expensive option is to take 500 mg of acyclovir five times a day. Most people find it easier to take 1000 mg of valacyclovir three times a day, and it seems to work better, at least for Bell’s palsy. You can also take 500 mg of famciclovir three times a day, which seems to work better than acyclovir.
Antiviral treatment is usually given for 7 to 10 days. However, some studies have shown that facial nerve axons continue to degenerate up to 21 days after paralysis starts, so antiviral treatment should be given for 21 days.
High doses of corticosteroids, such as 60 mg of prednisone every day for 21 days, are often given as well. This is done to prevent acute adrenal insufficiency. Corticosteroids can cause a number of side effects, such as irritability, insomnia, gastroesophageal reflux, and high blood sugar. Patients should be told about these side effects.
Patients with diabetes who are fragile may not be able to handle these high doses of steroids, so they should adjust their hypoglycemic medications as needed. In some cases, it may be better to use insulin for a short time than to stop taking steroids, because glucocorticoids and antiviral drugs work better together than antivirals alone.
Treatment should begin as soon as possible, but patients who don’t show up for care until a week after the onset can still benefit from treatment.
Complications
Ramsay Hunt syndrome is best treated with drugs by a primary care provider, but a specialist consultation with a doctor who has experience with acute facial paralysis may be helpful.
A facial plastic surgeon or otolaryngologist may know more about how to treat Ramsay Hunt syndrome than a general practitioner, and they may also have easier access to audiometry and flexible fiberoptic laryngoscopy. A neurologist can also help diagnose cranial neuropathies and treat chronic neuralgia. For people with complete hemifacial paralysis, he or she may be able to do electrodiagnostic testing.
With a slit-lamp exam and fluorescein dye, an ophthalmologist can check the health of the cornea. If needed, both the ophthalmologist and the otolaryngologist should be able to put an eyelid weight in place. During long-term high-dose steroid use, blood glucose levels may need to be managed by an internist or endocrinologist.
Lastly, some patients will need to see a specialist in mental health to help them deal with mood problems and anxiety that are caused by facial dysfunction.
Be the first to comment